Covid-19: The third wave

The absence of all-island cooperation is limiting the ability to successfully control the Covid-19 pandemic in Ireland. Meanwhile, a cyclical policy of suppressing SARS-CoV-2 through public health restrictions continues to stifle society and the economy. agendaNi assesses recent Covid-19 developments.
A failure to achieve consensus on the harmonisation of the Covid-19 response across the island has served to undermine the effectiveness of public health measures in both jurisdictions. Locally, the Northern Ireland Executive has behaved with dysfunction. A reluctance on behalf of some Executive parties to diverge from the British response to the crisis has collided with a rejection of that same response by others. The ensuing horse trading on public health restrictions against the interests of lobby groups created a significant delay in recognising the ongoing crisis in the health system.
For instance, in mid-November 2020, the DUP utilised a cross-community veto to thwart a proposed two-week extension to public health restrictions. Indeed, one month previously, the party had criticised the Executive’s latest restrictions and acceded to the democratic will of its government partners with apparent reluctance.
Meanwhile, the introduction of successive restrictions, some euphemistically referred to as a ‘circuit breaker’, and lockdowns has served to diminish public trust and confidence. This is exacerbated by poor communication from and an obvious lack of coherence within the Executive.
Consequently, while each winter in Northern Ireland heralds an annual crisis in the health and social care system, winter 2020/2021 is a different animal. From December 2020, hospitals across Northern Ireland have consistently exceeded capacity while the challenges posed by an exponential increase in Covid-19 transmission have been inadvertently compounded by infection control measures and staff sickness.
Zero Covid alternative
Speaking with agendaNi in July 2020, President of the Epidemiology and Public Health section of the Royal Society of Medicine Gabriel Scally outlined: “We will either get to zero cases on the island and relax many restrictions or, if we don’t have effective border controls and a good testing regime, we will have to wait for a vaccine.”
During that same month, the Northern Ireland Assembly Committee for Health considered the A Better Way to Go: Towards Zero Covid report from the Independent Scientific Advisory Group for Emergencies (Independent SAGE). The Committee agreed to forward a copy of the report to the Health Minister, asking him to adopt a ‘zero Covid’ objective, and to seek his views on each of the recommendations.
The zero Covid approach, as adopted by Australia, New Zealand, Taiwan and Vietnam, seeks to effectively eliminate the SARS-CoV-2 virus within a defined geographic entity. The absence of community transmission for a period of time enables the safe reopening of the economy. While there would still be a potential for imported cases, these could be controlled.
Rolling lockdowns
While zero Covid has remained politically unobtainable in Ireland, Gabriel Scally’s analysis has proved to be true. In the absence of zero Covid, recurrent waves of transmission and rolling lockdowns have filled the vacuum. Both north and south, the administrations on the island have sought to utilise increasingly ineffective lockdowns as their primary tool to mitigate the pandemic, hitherto controlling it just within the capacity restraints of the two healthcare systems.
In other words, current policy seeks the suppression of Covid-19 to an ‘acceptable level’, enabling the economy to reopen between surges in transmission while awaiting vaccination rollout. One public health measure which has facilitated this strategy has been the ‘lockdown’ concept.
Such a strategy has proved costly in the UK and Ireland. Speaking as early as May 2020, the Executive Director of WHO Health Emergencies Programme, Michael Ryan, warned against easing public health restrictions too soon and reopening the economy too quickly, suggesting that it could lead to a “vicious cycle” of economic and health catastrophe.
“This is what we all fear; a vicious cycle of public health disaster followed by economic disaster followed by public health disaster followed by economic disaster. If you reopen in the presence of a high-degree of virus transmission, then that transmission may accelerate,” he said.
Similarly, at the outset of the pandemic, Ryan advised that: “We have got to be able to show that we can go after the virus because lockdowns alone will not work.” This was supported by WHO Director General Tedros Adhanom Ghebreyesus who stated: “So-called lockdowns can help to take the heat out of a country’s epidemic, but they cannot end it alone. Countries must now ensure they can detect, test, isolate and care for every case, and trace every contact.”
Again, speaking with The Spectator’s Andrew Neil in October 2020, David Nabarro reiterated: “We in the World Health Organisation do not advocate lockdowns as a primary means of control of this virus. The only time we believe a lockdown is justified is to buy you time to re-organise, regroup, rebalance your resources, protect your health workers who are exhausted, but by and large, we’d rather not do it.
“We really do appeal to all world leaders: stop using lockdown as your primary control method. Develop better systems for doing it. Work together, and learn from each other.”
During the same month, The Lancet published a letter titled the “scientific consensus on the Covid-19 pandemic”. In the letter, signed by 80 public health experts and doctors (and subsequently signed by over 4,000 more), the rationale for lockdowns is acknowledged as being about slowing the spread of the virus and ensuring that health systems are not overwhelmed. It identifies Japan, Vietnam and New Zealand as having demonstrated that “robust public health responses can control transmission, allowing life to return to near-normal”.
While conceding that lockdowns have been disruptive, both socially and economically, the letter asserts that “these effects have often been worse in countries that were not able to use the time during and after lockdown to establish effective pandemic control systems”.
“In the absence of adequate provisions to manage the pandemic and its societal impacts, these countries have faced continuing restrictions. This has understandably led to widespread demoralisation and diminishing trust,” the letter emphasises, concluding: “The evidence is very clear: controlling community spread of Covid-19 is the best way to protect our societies and economies until safe and effective vaccines and therapeutics arrive.”
All-island cooperation
If zero Covid is to be pursued as a realistic alternative to cycles of lockdown, it must be achieved by all-island consensus. For instance, as exposed by the Christmas travel ban in the Republic, any effort to enforce a rigid quarantine upon arrival strategy akin to that in New Zealand (where borders are closed to most visitors and all arrivals are tested and quarantined for 14 days) must be pursued on an all-island basis to prevent circumvention using ports in an alternative jurisdiction.
In December 2020, when the Republic introduced a 48-hour travel ban (subsequently extended) to and from Great Britain, the Executive stopped short of a similar embargo, instead advising against non-essential travel. Consequently, in response to the Irish Government’s decision and the subsequent predictable surge of people circumventing the ban via northern ports, the Executive’s Health Minister, Robin Swann MLA suggested: “It left us as the funnel or as the avenue of getting back in.”
The lack of meaningful collaboration is conspicuous. Indeed, Swann had previously intervened in July 2020 and again in September, through a series of four letters to the Republic’s Health Minister Stephen Donnelly TD, relating to the data of passengers travelling north via Dublin Airport. However, Swann received no written response from his southern counterpart.
Already, in October 2020, Taoiseach Micheál Martin TD has rejected the zero Covid approach as being unrealistic. “Given our geographic location and proximity to Britain and mainland Europe, and with two jurisdictions on our island, the advice of NPHET is, and our view as a Government is that this is simply not a realistic option,” he said.
“33,863 vaccinations in a short space of time is a significant achievement for Northern Ireland. We are continuing to lead the way in delivering vaccines to our most vulnerable and our frontline workers.”
— Health Minister Robin Swann MLA
Lingering crisis
The Covid crisis will linger long into 2021. In the meantime, an already weakened health system is paralysed by rising transmission rates, forcing hospitals to operate beyond capacity, decimating health and social care staffing and undermining non-Covid care.
From 26 December 2020, a six-week lockdown was imposed, with a review scheduled for 23 January 2021. A curfew was also implemented between 20:00 and 06:00 until 2 January with all retail, hospitality and leisure closed between those hours.
Welcoming the consensus within the Executive, the Health Minister said: “The evidence before us was clear that decisive intervention was required to prevent the growing tide of Covid-19 cases overwhelming out health service, with catastrophic consequences.”
Vaccination roll-out
Some hope emerged when the first Pfizer/BioNTech Covid-19 vaccination was administered to nurse Joanna Sloan on 8 December 2020. The initial phase of the vaccination programme focused on care home residents and staff, alongside HSC staff in direct contact with vulnerable patients. Second doses of the vaccine began on 29 December, by which point 8,940 care home residents, 10,484 care home staff and 14,259 HSC had received the vaccine.
The Health Minister said: “33,863 vaccinations in a short space of time is a significant achievement for Northern Ireland. We are continuing to lead the way in delivering vaccines to our most vulnerable and our frontline workers.”
Welcoming the approval of the Oxford/AstraZeneca Covid-19 vaccine the following day, Swann stated: “The vaccine programme will transform the situation but that will take time. Between now and then, we need another big push to get through these next few months. We can all play our part in supporting the health service and in protecting each other from Covid-19.”
The initial phase of the Oxford/AstraZeneca Covid-19 vaccination programme began on 4 January 2021, beginning with those aged 80 years and over and determined by clinical vulnerability factors.
Latest restrictions
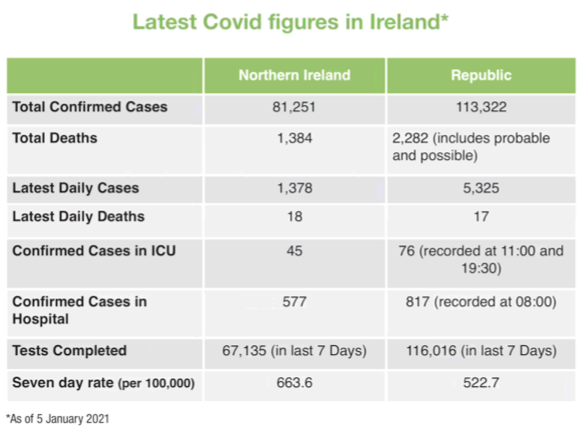
Now, the latest Covid-19 statistics indicate that Northern Ireland has a seven day incidence rate of 663.6 per 100,000 (as of 4 January 2021) compared to the Republic’s 14 Day Incidence Rate of 245.6 per 100,000 (as of 28 December 2020).
As the two jurisdictions on the island enforce their latest respective rounds of lockdown, it seems unlikely that the cycle will be broken. There is, however, some consensus on the response required in the latest phase of the crisis. First Minister Arlene Foster MLA stated: “The advice coming to us is that we will need to take action and that we’ll need to take action very quickly.” Likewise, deputy First Minister Michelle O’Neill MLA tweeted: “Urgent decisive action is required to respond.”