Health inequality remains wide in Northern Ireland

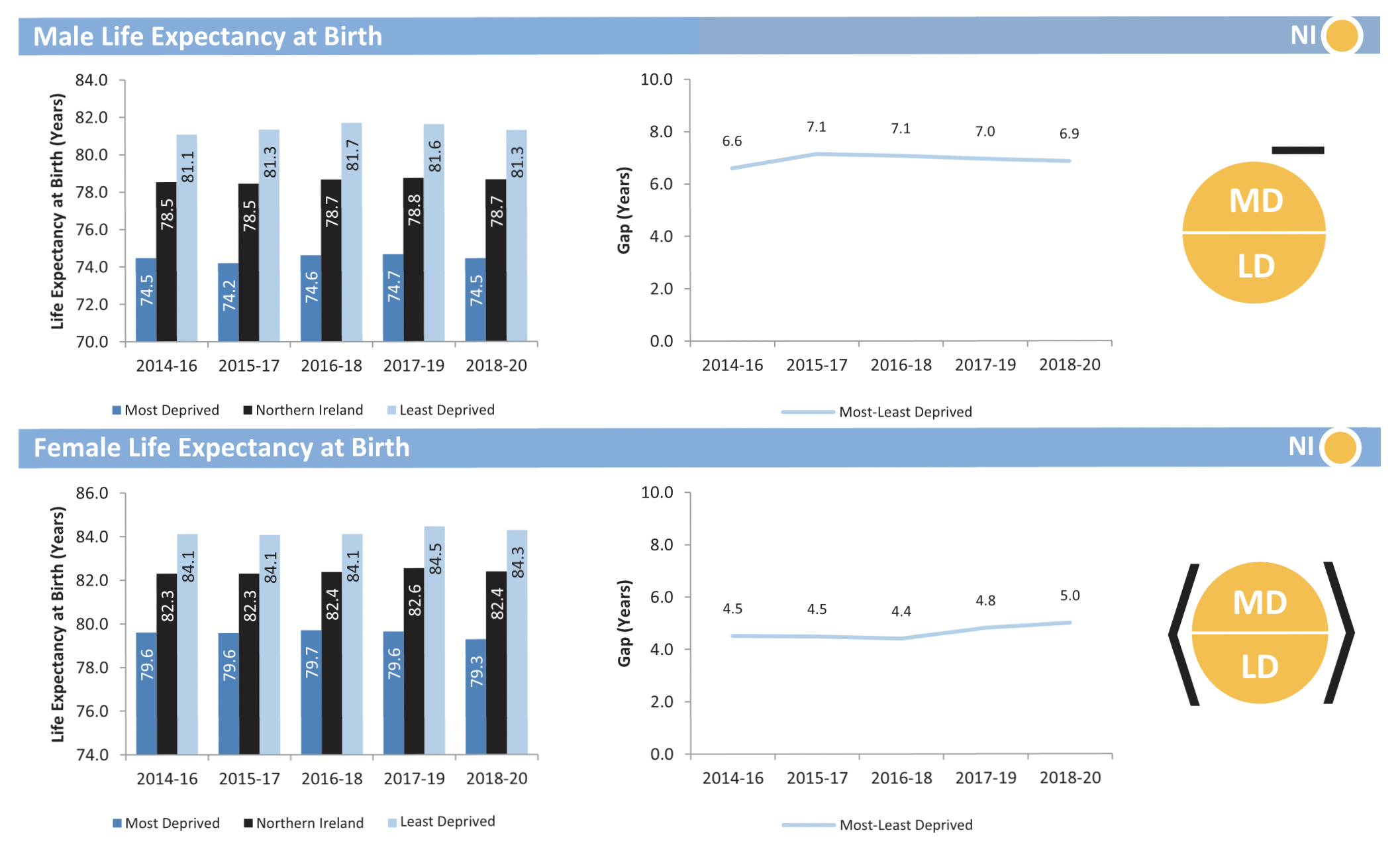
A report by the Department of Health has found that, between 2018 and 2020, the gap in life expectancy between the region’s most prosperous areas and its most economically deprived areas remained high, with a gap of almost seven years for men and five years for women.
The report is a study which examines the impact of social deprivation on health outcomes, determining whether there is a correlation between economic prosperity by area and health outcomes in each area.
The regional equality gaps take this into account by measuring the health outcomes of the 20 per cent most economically deprived areas with those of the 20 per cent most economically prosperous areas in Northern Ireland.
Diseases
Having covered the year 2020, the study was able to take account of some of the deaths from Covid-19 in Northern Ireland, and found that there was a relatively wide health inequality gap, with deaths from Covid-19 more prevalent in the least economically prosperous areas of Northern Ireland to the tune of 25 per cent.
The report additionally found that the largest inequality gap was observed for admissions due to respiratory diseases, with the rate in the most deprived areas more than double that of the least deprived, for all ages and for those aged under 75 years.
Furthermore, although the gap for cancer remained the same, rates went up for people of all economic backgrounds throughout the period.
Life expectancy gap
The report finds that, between the periods 2014-16 and 2018-20, there was no change in male healthy life expectancy in Northern Ireland’s least deprived areas, however there was an improvement in the most deprived areas. Over the same period, there was no change in female healthy life expectancy across all areas.
Life expectancy for citizens who have no disabilities increased in Northern Ireland for both males and females, although there was no notable change in most and least deprived areas or the deprivation gap for either gender.
“Premature mortality rates either decreased over the aforementioned period in the most and least deprived areas or showed no notable change,” the report states.
It continues: “The exception to this was preventable mortality, which increased in Northern Ireland, however, large inequality gaps continue to persist, with the rate of respiratory mortality among under 75s in the most deprived areas over three-and-a-half-times that in the least deprived.”
Across indicators of premature mortality, the inequality gaps remained fairly static, with a few exceptions where gaps narrowed, most notably treatable mortality.
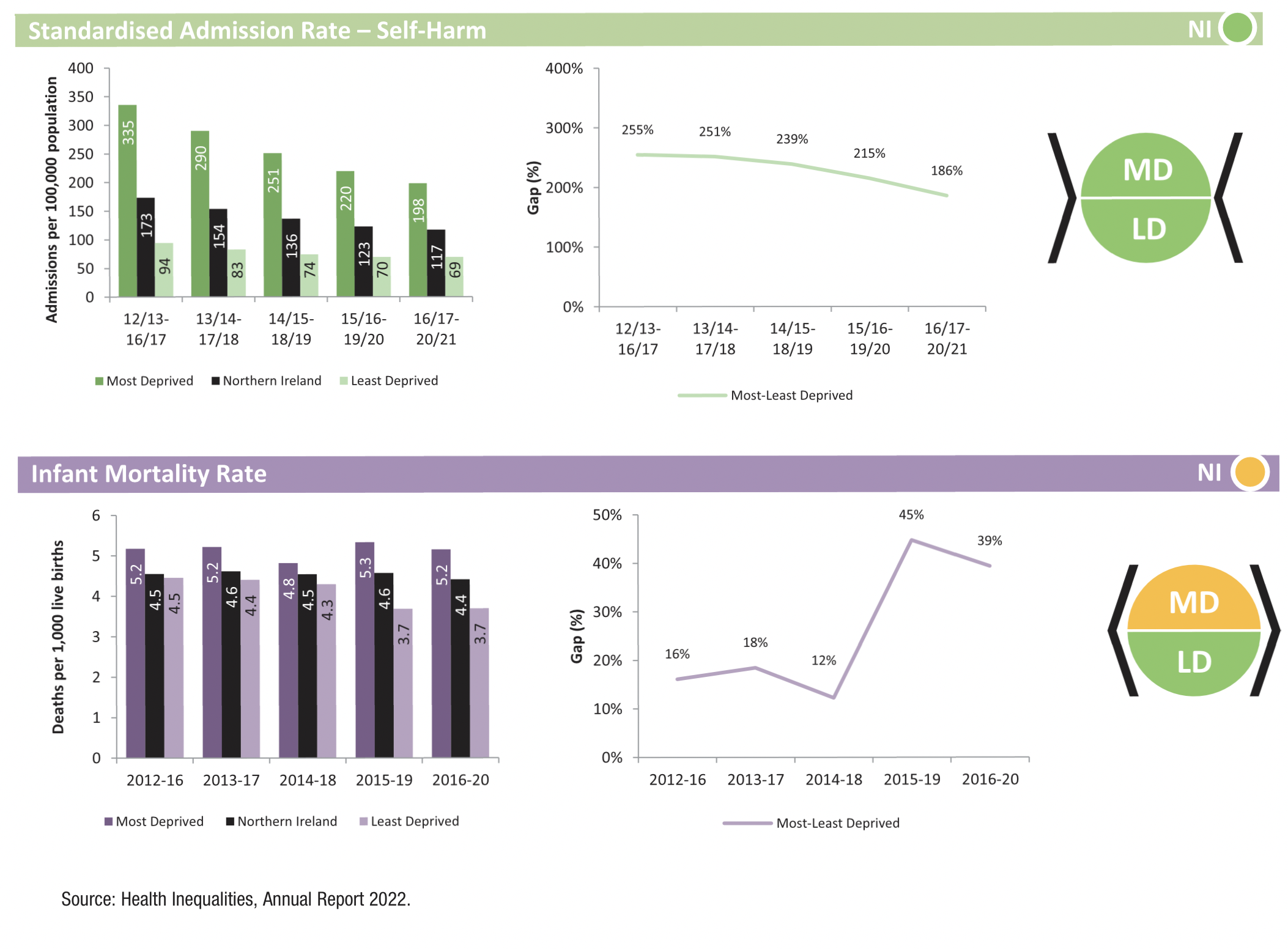
The infant mortality gap remained fairly static, but likewise an infant born in one of Northern Ireland’s economically deprived areas is 39 per cent more likely to die than one born in an economically prosperous area.
Mental health inequality
Although the mental health equality gap reduced in the period between 2018 and 2020, compared with the period between 2014 and 2016, the gap remains large. The study found that people from an economically deprived area are 186 per cent more likely to have self-harmed, compared with someone from an economically prosperous area.
Incidents of anxiety and low mood remained virtually identical in all areas, with an equality gap of 67 per cent recorded between Northern Ireland’s most deprived and prosperous areas.
The report further found that indicators related to alcohol and drugs showed among the highest levels of health inequalities in the region with rates in the most deprived areas over four-and-a-half-times that in the least deprived for drug related mortality and four-times that for alcohol specific mortality.
Furthermore, there was a 306 per cent equality gap in alcohol-related illness. This figure was recorded over a four year period between 2016 and 2020.