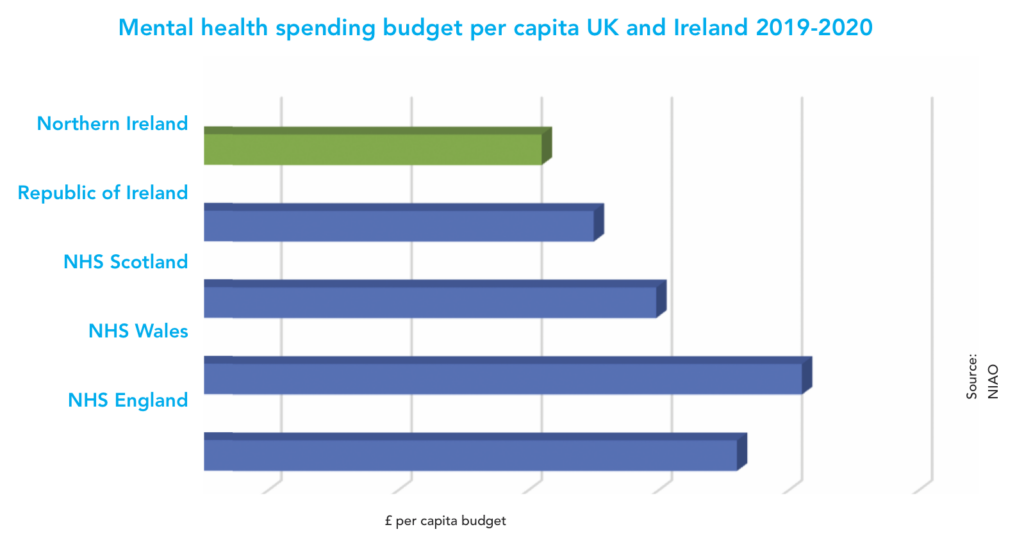
Northern Ireland’s Comptroller and Auditor General is “unable” to say whether the £300 million being spent on mental health services in the region is providing value for money.
Dorinnia Carville said that in the absence of an identified outcome framework and appropriate measures to assess whether services are making a difference in terms of improving mental health, the Northern Ireland Audit Office (NIAO) was unable to conclude whether mental health services in Northern Ireland are providing value for money.
The NIAO’s critical report comes at a time of mental health crisis in Northern Ireland, where increased demand and spiralling waiting lists are being underserved by the absence of agreed Executive funding for a new 10-year Mental Health Strategy.
Planned actions for the strategy to 2031 were costed at an estimated £1.2 billion but no Executive-agreed funding has ever been allocated. The first two successive annual delivery plans have delivered funding well short of what was originally outlined.
The Comptroller and Auditor General says that without dedicated long-term funding, the delivery of the strategy and achievement of its vision for mental health “remain at risk”.
Work done by the London School of Economics and the Mental Health Foundation in February 2022 put a conservative estimate of £3.4 billion in a given year on the overall cost of mental ill-health in Northern Ireland, recognising costs of not only the personal impact of mental ill-health and to those around them, but also the wider societal impacts of costs of care, treatment, and lost production.
Perhaps most strikingly, despite the current and future expenditure needed to address the mental health crisis, the NIAO points to an incomplete picture of mental health provision, based on current data.
Highlighting a lack of regional standardisation and a fragmented information technology infrastructure, the NIAO pinpoints that available information is focused on health trust activity, but that no detail is available in relation to mental health services in primary care. Similarly, it states, there is a lack of information on services provided by the community and voluntary sector (other than as an integral part of Trust services, provided under contract).
Concluding that the Department and trusts remain “unsighted as to whether the services provided represent value for money”, one of the NIAO’s priority recommendations is for the production of a data strategy, including use of an appropriate outcomes measurement framework.
While an outcomes framework is being progressed by the Department, its implementation timeframe is tied to the information technology systems currently scheduled not to be fully brought into use until March 2025.
Crisis
In the meantime, Northern Ireland continues to have the highest prevalence of mental health problems of any region of the UK, with the size of the gap emphasised by the fact that mental ill-health rates are around 25 per cent higher than in England. Despite this, planned expenditure on mental health (£1.2 billion over 10 years as set out by the Mental Health Strategy funding plan) for Northern Ireland represents around 2 per cent of the Department of Health’s estimated £6 billion annual budget over the decade. Comparatively, England and Wales dedicate around 13 per cent of their annual health budget to mental health services.
The recently published Mental Health Strategy Delivery Plan for 2023/24 allocated £5.5 million to implementation of the Mental Health Strategy’s ambitions but acknowledged that the allocation “is less than the requirements”.
Recent figures released by the Department of Health showcase the extent of the service crisis in Northern Ireland. On 30 June 2023, there were 2,251 total waits for a Child and Adolescent Mental Health Service (CAMHS) assessment in Northern Ireland, of which more than half (1,205) were waiting more than the targeted nine weeks.
In her conclusions, the Comptroller and Auditor General says: “In the absence of an identified outcome framework and appropriate measures to assess whether services are making a difference in terms of improving mental health, we are unable to conclude on whether mental health services in Northern Ireland are providing value for money.”
As well as recommendations for the creation and implementation of a data strategy, other recommendations issued by the NIAO include the needs to secure adequate and sustained funding for the implementation of the strategy over its lifetime, adding that failure to do so would “jeopardise the achievement of its long-term vision for mental health and run the risk that, like Bamford before it, necessary reform and improvement is curtailed or delayed as a result of a lack of commitment to prioritise and adequately fund implementation”.
Further to this, Carville says that aligning funding levels in Northern Ireland with those elsewhere will require the Department of Health to establish a long-term funding ambition for mental health services “together with stepped interim targets aimed towards its achievement”.