New thinking needed for health finance
 Speaking at agendaNi’s infrastructure seminar, Mark Hellowell predicted that increased demand and constrained finance will prompt governments to look for new private sector sources of funding for healthcare.
Speaking at agendaNi’s infrastructure seminar, Mark Hellowell predicted that increased demand and constrained finance will prompt governments to look for new private sector sources of funding for healthcare.
Public finance alone cannot meet the growing demands of health services, according to Mark Hellowell. The University of Edinburgh academic lectures in global health policy and spoke at agendaNi’s seminar on the future of infrastructure delivery.
“One of the distinctive dimensions of social infrastructure investment is the extent to which you’re reliant on public sector funding – state funding – of the assets over the long term,” he remarked. However, there were “pretty significant constraints” on the public sector’s ability to pay over the coming years. Political will for large new investments was questionable but so too was whether new, large scale investments were needed. A high level of investment was directed into the UK’s health infrastructure between 2000 and the financial crash.
The stronger argument is that there is a substantial need from a cost-benefit perspective for additional investment.
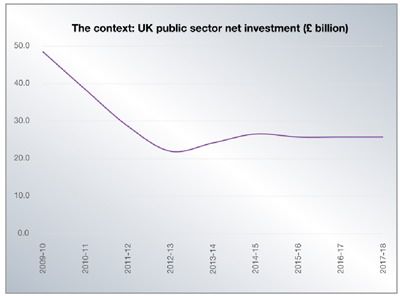
There is an “emerging gap” between ministerial rhetoric on public investment and the implied budgets that it would involve. As the table indicates, total public sector net investment peaked in 2009-2010 before a major reduction in absolute terms and also relative to GDP. This downward trend is set to continue.
“Relying on public capital to maintain an adequate stock of infrastructure – and perhaps even invest in the additional infrastructure requirements that we have in healthcare – may not actually be a viable solution,” Hellowell commented. “We might need to look beyond traditional sources of financing.”
For private financing, there will still be a limit on what the public sector can pay for new infrastructure. Healthcare spending peaked at 8 per cent of UK GDP in 2009, now stands at just over 7 per cent and is officially projected to fall to 6.6 per cent by 2020. This would bring it back down to 2003 levels.
In this unprecedented situation, the NHS will face substantial budgetary challenges across the UK. “It’s very, very difficult to exert long-term downward pressure on healthcare costs,” he explained, “given changing technology, given changing demographic patterns [and] given rising relative prices.”
Ministers claim that health has been protected against austerity. Indeed, between 2010 and 2016, overall UK Government health spending is expected to grow by 2.9 per cent compared to reductions of 10.1 per cent in education, 25.5 per cent in the Home Office budget, and 29.5 per cent in the local government subvention.
That said, it is not clear whether this can be sustained in the next Parliament. The Institute for Fiscal Studies has suggested that ring-fencing health will be very difficult regardless of which party wins the next general election. Decisions at Westminster will still have an impact on devolved administrations’ budgets through the Barnett formula.
The number of project finance initiative schemes in the UK rose from one in 1995 to 66 in 2000. By the time of the financial crisis, around £4 billion of contracts were being signed every year. Since then, that value has fallen to £1 billion or less.
Policy during the financial crisis focused on the supply side. Early on in the crisis, the bond market was disrupted by the collapse of major insurers. This led to an increased reliance on banks whose liquidity was also constrained and international regulations now require banks to set aside more capital against riskier assets.
Attention is now turning to the more significant constraints on the demand side. Firstly, since 2010, there is a “huge amount of political uncertainty” about using private finance in the public sector. The Private Finance 2 model has been implemented, with a focus particularly on education, but its long-term future is unclear.
 Hellowell saw a degree of convergence between the UK and Scottish PPP models:
Hellowell saw a degree of convergence between the UK and Scottish PPP models:
• less risk being transferred to the private finance;
• keeping services in-house;
• controlling departments’ ability to enter into projects with substantial future liabilities;
• de facto regulation of returns (the non-profit distributing model);
• a focus on reducing gearing or leverage; and
• investment of public sector equity capital (to reduce risk and cost).
A lot of policy work and negotiation had taken place and the pipelines of work are “promising” but there is “not a huge amount of deal-flow.” He reiterated that government capital is likely to be very constrained and PFI-based PPPs will have their own constraints while the level of healthcare demand will continue to rise.
The “blue sky thinking” about tackling that challenge includes engaging private sector providers to deliver public healthcare free at the point of delivery – as happens in England. The providers can bring in their own capital to deliver their assets, independently of the government balance sheet.
Hellowell stated: “I genuinely do think that we’re in a period where the constraints on NHS spending are so unprecedented and so challenging for policy-makers to meet that this kind of structural change in the healthcare system is probably non-discretionary.”
As a result, new forms of equity and debt capital may potentially be sought out to provide the level of investment that the Health Service needs.